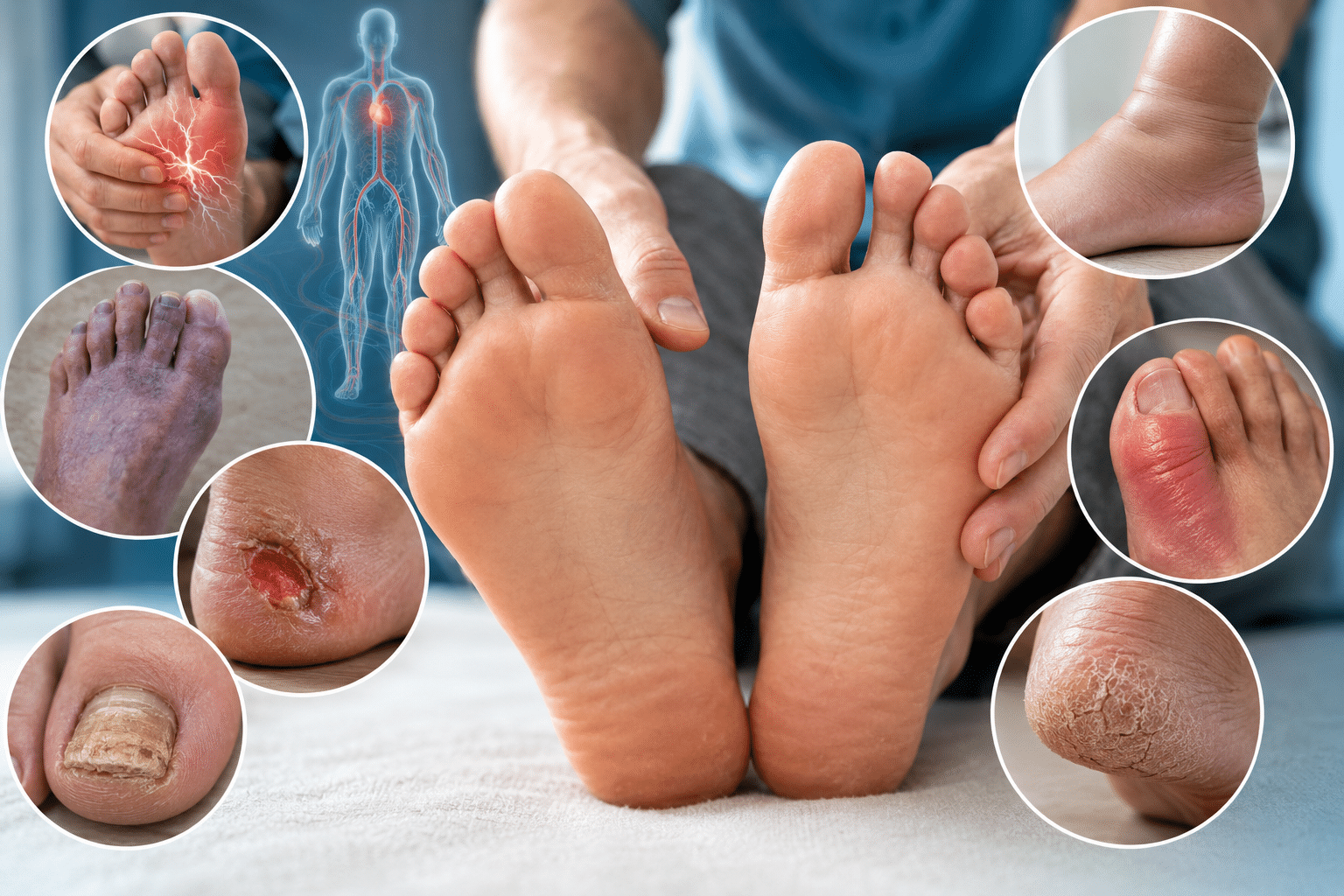
Signs Your Body May Be Developing Diabetes
Part 2 of 2 · Early detection, testing & what to do next
Why Recognizing Diabetes Symptoms Early Matters
The clinical significance of early detection cannot be overstated. When type 2 diabetes or prediabetes is identified before significant damage has occurred to the body’s tissues and organs, interventions — including dietary changes, increased physical activity, and in some cases medication — can dramatically reduce the risk of progression and complication. The CDC’s National Diabetes Prevention Program, for example, has documented that lifestyle changes in people with prediabetes can reduce the risk of developing type 2 diabetes by as much as 58 percent over three years, or 71 percent among adults over 60.
When left undetected or unmanaged, chronically elevated blood glucose progressively damages blood vessels and nerves throughout the body. The long-term complications of uncontrolled diabetes include cardiovascular disease, kidney disease (diabetic nephropathy), vision loss and blindness (diabetic retinopathy), lower limb nerve damage (peripheral neuropathy), and an elevated risk of foot ulcers and amputations. These are not inevitable outcomes — they are complications strongly associated with poor blood sugar control over time, which is precisely why catching the earliest warning signs and confirming or ruling out diabetes through blood testing is so valuable.
When to See a Doctor About Diabetes Symptoms
Medical organizations including the NHS, the ADA, and the Mayo Clinic consistently advise that any individual who notices persistent symptoms associated with high blood sugar — particularly the combination of increased thirst, frequent urination, and unexplained fatigue — should seek an evaluation without delay. A single blood test can provide rapid, definitive information about current blood glucose levels, and the appointment need not be complex or time-consuming.
For individuals without current symptoms, the CDC and U.S. Preventive Services Task Force (USPSTF) recommend screening for prediabetes and type 2 diabetes beginning at age 35 for adults who are overweight or obese. Those who have any of the risk factors outlined above may benefit from earlier or more frequent screening. Pregnant individuals should typically be screened for gestational diabetes between weeks 24 and 28 of pregnancy, as gestational diabetes increases the long-term risk of developing type 2 diabetes after delivery.
In situations where symptoms of very high blood glucose develop rapidly and include severe vomiting, abdominal pain, difficulty breathing, confusion, or loss of consciousness — signs that may indicate diabetic ketoacidosis (DKA), a serious complication predominantly associated with type 1 diabetes — emergency medical care should be sought immediately. DKA is a life-threatening condition that develops when the body begins breaking down fat rapidly due to insufficient insulin, producing acidic ketone bodies in the bloodstream.
Blood Sugar Testing: What the Numbers Mean
Understanding blood glucose testing results can help individuals contextualize their own health data. The three most common diagnostic tests for diabetes are the fasting plasma glucose test, the A1C test (also called the glycated hemoglobin test), and the oral glucose tolerance test. Each measures blood glucose in a slightly different way and provides different windows into how the body handles sugar over varying timeframes.
According to the ADA’s current diagnostic criteria, a fasting blood glucose level below 100 mg/dL is considered normal; between 100 and 125 mg/dL indicates prediabetes; and 126 mg/dL or higher on two separate tests confirms a diagnosis of diabetes. For the A1C test, which measures average blood glucose levels over the prior two to three months, results below 5.7 percent are normal, 5.7 to 6.4 percent indicates prediabetes, and 6.5 percent or above on two separate occasions confirms diabetes. A healthcare provider is best placed to interpret these results in the full context of an individual’s medical history and other clinical findings.
Frequently Asked Questions About Diabetes Warning Signs
The earliest and most commonly reported signs include increased thirst, more frequent urination (particularly at night), and a sense of fatigue that is not explained by activity levels. In type 2 diabetes, these symptoms can be mild enough that they go unnoticed for extended periods. In type 1 diabetes, onset tends to be more abrupt, with symptoms often appearing within days to weeks. Any persistent combination of these symptoms warrants a blood glucose test.
Yes. Prediabetes almost never causes symptoms, and many people with early-stage type 2 diabetes have no noticeable symptoms at all. The CDC estimates that over 80 percent of people with prediabetes are unaware of their condition. This is why routine blood glucose screening is recommended for adults with risk factors, even in the absence of symptoms.
Diabetes is confirmed through blood testing, not symptoms alone. The most commonly used tests are the fasting plasma glucose test, the A1C (glycated hemoglobin) test, and the oral glucose tolerance test. A healthcare provider will typically require at least two abnormal results from the same test or two different tests before making a formal diagnosis, unless symptoms are severe and a single very high reading is obtained.
Not necessarily. Tingling or numbness in the extremities — a condition related to peripheral neuropathy — can be caused by several conditions beyond diabetes, including vitamin B12 deficiency, carpal tunnel syndrome, poor circulation, and certain medications. However, when tingling appears alongside other diabetes-associated symptoms such as increased thirst, frequent urination, or fatigue, it strengthens the case for blood glucose testing. A healthcare provider can conduct the appropriate evaluation to determine the underlying cause.
For prediabetes, evidence-based lifestyle interventions — including sustained weight loss of 5 to 7 percent of body weight and at least 150 minutes of moderate physical activity per week — have been shown by the CDC’s National Diabetes Prevention Program to reduce the risk of progression to type 2 diabetes by up to 58 percent. Some people with early type 2 diabetes achieve normal blood sugar levels through significant lifestyle changes, though whether this constitutes true reversal or sustained remission is still a subject of clinical discussion. Type 1 diabetes cannot currently be prevented or reversed.
Taking Action Before Diabetes Takes Hold
The body rarely falls silent when something is going wrong — it offers clues, even when those clues are easy to rationalize away. The persistent thirst that seems like nothing more than a hot day, the fatigue that feels like ordinary stress, the slow-healing cut that is blamed on aging — these small signals, taken together, may be telling a more significant story. Diabetes is among the most prevalent chronic diseases in the world, yet it is also among the most responsive to early intervention. Knowing what to look for, understanding the risk factors that heighten personal vulnerability, and seeking a simple blood test when something does not feel right are accessible, genuinely powerful steps. The gap between prediabetes and diabetes is not a foregone conclusion — it is a window, and for many people, there is still time to act within it.