Signs Your Body May Be Developing Diabetes
Recognizing early warning symptoms can make a critical difference — here is what to watch for and when to seek medical advice.
Developing diabetes is a process that often unfolds quietly, with the body sending subtle distress signals long before a formal diagnosis is made. The signs your body may be developing diabetes can be easy to dismiss as ordinary fatigue, the effects of a busy lifestyle, or simply getting older — yet heeding these early warnings can substantially alter the course of the condition. According to the Centers for Disease Control and Prevention (CDC), more than 38 million Americans have diabetes, and a further 98 million adults have prediabetes, a state in which blood sugar levels are elevated above normal but not yet high enough to qualify as type 2 diabetes. Crucially, the CDC estimates that more than 80 percent of people with prediabetes are unaware of their condition. Understanding what these warning signs look like — and why they occur — is among the most important steps any person can take toward protecting their long-term health.
Understanding the Two Primary Types and How They Differ
Before exploring the specific symptoms, it is helpful to understand that diabetes is not a single, uniform disease. Type 1 diabetes is an autoimmune condition in which the body’s immune system mistakenly attacks and destroys the insulin-producing beta cells in the pancreas. Because insulin production is severely reduced or eliminated, glucose cannot enter cells for energy use and instead accumulates dangerously in the bloodstream. Type 1 diabetes can develop at any age, though it frequently appears in children and young adults; its onset can be rapid, with pronounced symptoms emerging over days to weeks.
Type 2 diabetes, the far more prevalent form, develops when the body either does not produce enough insulin or does not use the insulin it produces effectively — a condition known as insulin resistance. Unlike type 1, type 2 diabetes typically develops gradually, often over years, and its early signs can be subtle or even absent. Prediabetes, which precedes type 2 diabetes, rarely causes noticeable symptoms at all, which is why routine blood glucose screening is recommended for individuals with risk factors, particularly those over the age of 35.
Editorial categorization — type comparison for informational context
Early Warning Signs and Symptoms of Developing Diabetes
Both the Mayo Clinic and the American Diabetes Association (ADA) identify a cluster of warning symptoms that individuals should be aware of. These symptoms arise primarily because elevated blood glucose — a condition known as hyperglycemia — places physiological stress on multiple organ systems simultaneously. Not every person will experience every symptom, and some individuals with type 2 diabetes may have no symptoms at all in the early stages.
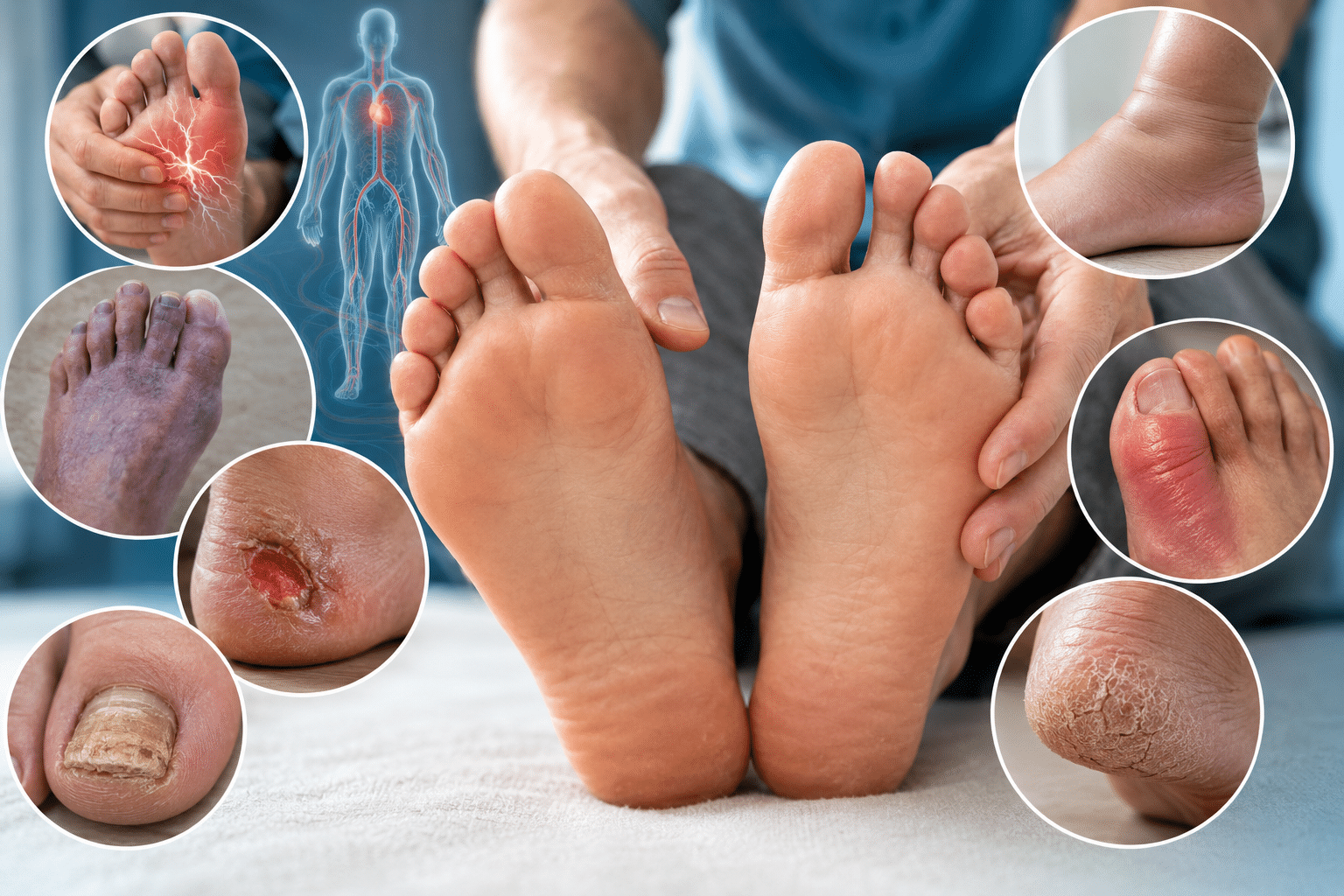
Skin Changes and Other Less Obvious Signs of High Blood Sugar
Beyond the well-known trio of thirst, urination, and hunger, the body can signal developing diabetes in less intuitive ways. Recurrent infections — particularly yeast infections, urinary tract infections, or skin infections — may point to an environment in which elevated blood glucose provides a favorable medium for bacterial and fungal growth. The American Diabetes Association notes that high blood sugar can suppress normal immune function, making it harder for the body to fight off pathogens that would otherwise be contained.
One particularly notable but sometimes overlooked skin change is a condition called acanthosis nigricans — darkened, thickened patches of skin that appear in body folds and creases such as the neck, armpits, and groin. According to the Mayo Clinic, acanthosis nigricans is often associated with insulin resistance and can be an early visible marker of prediabetes or type 2 diabetes, particularly in individuals who are overweight or have a family history of the condition. The affected skin takes on a velvety texture and a darker hue compared to surrounding areas.
Dry, itchy skin is another symptom that can accompany developing diabetes. Poor circulation caused by elevated blood glucose can reduce the skin’s ability to retain moisture, and nerve damage may impair the body’s normal sweat-regulating mechanisms. Additionally, cuts and wounds that take an unusually long time to heal — or minor infections that seem disproportionately persistent — merit attention as potential early signals of metabolic disruption.
Risk Factors That Can Accelerate Diabetes Development
Certain characteristics and lifestyle patterns are established risk factors for developing type 2 diabetes, according to the CDC and the World Health Organization (WHO). While the presence of these factors does not guarantee that diabetes will develop, they significantly raise the statistical likelihood and increase the importance of monitoring blood glucose levels and any symptoms that arise.
It is important to note that type 1 diabetes follows a different risk profile. It is not preventable in the same way that type 2 diabetes often is, and its development is driven by genetic and environmental factors that researchers are still working to fully understand. Individuals with a close family member with type 1 diabetes have a modestly higher risk of developing the condition themselves, though the absolute risk remains relatively low for most people.