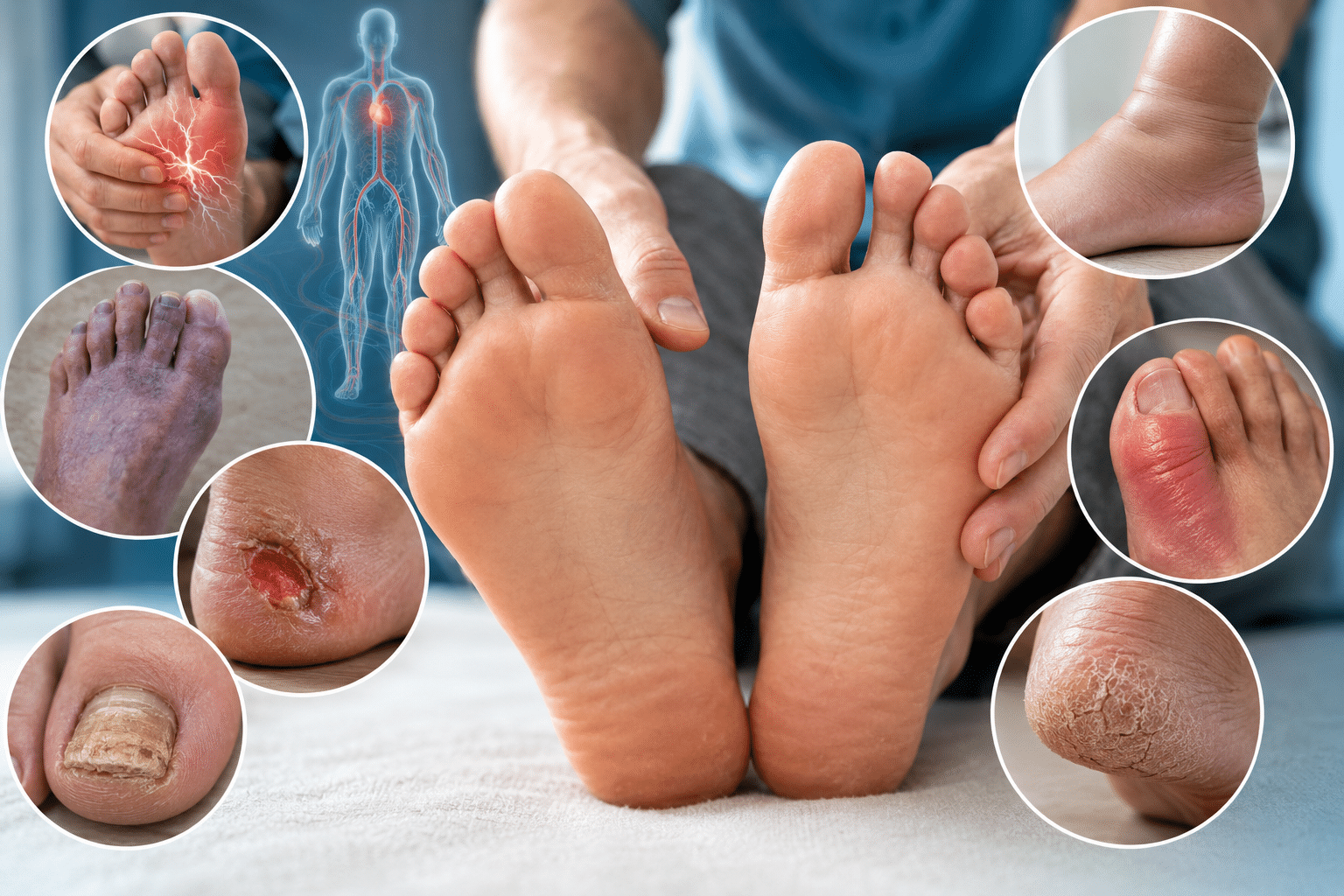
Type 2 diabetes is a chronic condition that develops gradually as the body becomes resistant to insulin or fails to produce enough of it to maintain normal blood sugar levels. Unlike sudden illnesses, the early stages often go unnoticed because the symptoms can be mild or easily mistaken for everyday fatigue or minor health issues. Recognizing these warning signs early is important, as it can allow individuals to take preventive steps before the condition progresses. Factors such as lifestyle habits, genetics, and overall health all play a role in determining risk, making awareness a key part of long-term health management.
Early Warning Signs Often Go Unnoticed

Many of the earliest signs of Type 2 diabetes are subtle and can easily be dismissed as normal fluctuations in energy or hydration. Individuals may notice slight changes in how they feel throughout the day, but these shifts are often attributed to stress, lack of sleep, or a busy schedule. Because these symptoms do not usually interfere significantly with daily life at first, they may go unrecognized for extended periods. This delay can allow blood sugar levels to remain elevated without intervention, increasing the risk of complications over time.
In addition, early symptoms may appear inconsistently, making them harder to connect to a larger issue. A person might experience fatigue one day and increased thirst the next without realizing the two could be related. These patterns often develop gradually, which further contributes to them being overlooked. Paying attention to recurring symptoms rather than isolated incidents can help identify potential concerns earlier and prompt further evaluation when necessary.
Increased Thirst and Frequent Urination

One of the more noticeable early signs of Type 2 diabetes is an increase in thirst accompanied by more frequent urination. When blood sugar levels rise, the kidneys work harder to filter and remove excess glucose from the bloodstream. This process draws more fluid from the body, leading to increased urine production. As a result, individuals may find themselves needing to use the restroom more often than usual, including during the night.
The loss of fluids through frequent urination can lead to dehydration, which in turn triggers persistent thirst. Even after drinking fluids, the feeling of thirst may not fully go away, creating a cycle that continues throughout the day. This combination of symptoms is often one of the earlier indicators that blood sugar levels may not be properly regulated. Recognizing this pattern and monitoring changes in hydration and bathroom habits can provide important clues about underlying metabolic issues.
Unexplained Fatigue and Low Energy

Persistent fatigue is another common sign associated with the early stages of Type 2 diabetes. When the body becomes resistant to insulin, glucose is not effectively transported into cells where it is needed for energy. As a result, even when enough food is consumed, the body may still feel low on energy. This can lead to ongoing tiredness that does not improve with rest or sleep.
In many cases, this fatigue may be accompanied by fluctuations in energy levels throughout the day. Individuals might feel especially tired after meals due to blood sugar spikes followed by rapid drops. This pattern can make it difficult to maintain focus and productivity, especially during routine tasks. Over time, this consistent lack of energy can impact daily life, making it an important symptom to recognize and evaluate in the context of overall health.
Changes in Vision and Slow Healing

Changes in vision can be an early indicator that blood sugar levels are not well controlled. Elevated glucose levels can affect the tiny blood vessels in the eyes, leading to temporary swelling in the lens. This can cause blurred vision or difficulty focusing, especially when shifting between distances. These changes may come and go, which can make them easy to dismiss as eye strain or fatigue rather than a sign of an underlying issue.
In addition to vision changes, the body’s ability to heal can also be affected. High blood sugar can impair circulation and reduce the efficiency of the immune system, slowing down the healing process. Cuts, bruises, or minor injuries may take longer than usual to recover, and infections may occur more frequently. Paying attention to how the body responds to injuries and whether healing seems delayed can provide useful insight into overall metabolic health.
Increased Hunger and Weight Changes

An increase in hunger, even after eating regular meals, can be another sign associated with developing Type 2 diabetes. When insulin is not functioning properly, glucose remains in the bloodstream instead of entering the cells where it is needed for energy. As a result, the body may signal hunger more frequently in an attempt to obtain the energy it is not effectively using. This can lead to overeating without a corresponding increase in energy levels.
Weight changes can also occur alongside increased hunger, although the direction of these changes may vary. Some individuals may experience weight gain due to excess glucose being stored as fat, particularly when calorie intake rises. Others may notice unintentional weight loss if the body begins breaking down muscle and fat for energy due to insufficient glucose use. These shifts in appetite and weight can reflect underlying metabolic imbalances and should be considered alongside other symptoms.
Risk Factors That Increase Your Chances

Several risk factors can increase the likelihood of developing Type 2 diabetes, many of which are related to lifestyle and genetics. A family history of diabetes can raise the risk, as genetic factors can influence how the body processes insulin. In addition, being overweight or having excess body fat, particularly around the abdomen, is strongly associated with insulin resistance. Physical inactivity can further contribute to this process, as regular movement plays a role in maintaining healthy blood sugar levels.
Age is another factor that can influence risk, as the body’s metabolism and insulin sensitivity may change over time. Certain health conditions, such as high blood pressure and prediabetes, can also increase the likelihood of progression to Type 2 diabetes. Environmental and demographic factors may play a role as well, with some populations experiencing higher rates of the condition. Understanding these risk factors can help individuals assess their own likelihood and take steps toward prevention through lifestyle adjustments and regular health monitoring.
Skin Changes and Other Physical Indicators

Certain visible changes in the skin can serve as early warning signs of insulin resistance and an increased risk of Type 2 diabetes. One of the most recognized indicators is the appearance of dark, velvety patches of skin, often found around the neck, underarms, or groin. This condition, known as acanthosis nigricans, is commonly associated with elevated insulin levels in the body. In addition to these patches, some individuals may notice an increase in skin tags, which are small, benign growths that can appear in areas where the skin folds.
Other physical indicators may include a higher frequency of infections and unusual sensations in the body. Individuals may experience recurring yeast infections or other skin-related infections due to changes in immune function and elevated blood sugar levels. Tingling, numbness, or a burning sensation in the hands and feet can also develop over time, which may be related to nerve involvement. These signs often appear gradually and may not seem immediately connected, but together they can point to underlying metabolic changes that should be evaluated.
Taking Action Before It Becomes a Diagnosis
Recognizing the signs of Type 2 diabetes risk is an important step toward protecting long-term health and preventing more serious complications. Many of these symptoms develop gradually and may not seem alarming on their own, which is why awareness and consistency in monitoring changes in the body are essential. Identifying patterns such as increased thirst, fatigue, or slow healing can help prompt earlier evaluation and intervention. With the right approach, including lifestyle adjustments and regular medical checkups, it is often possible to reduce risk and maintain better control over overall health before the condition progresses further.