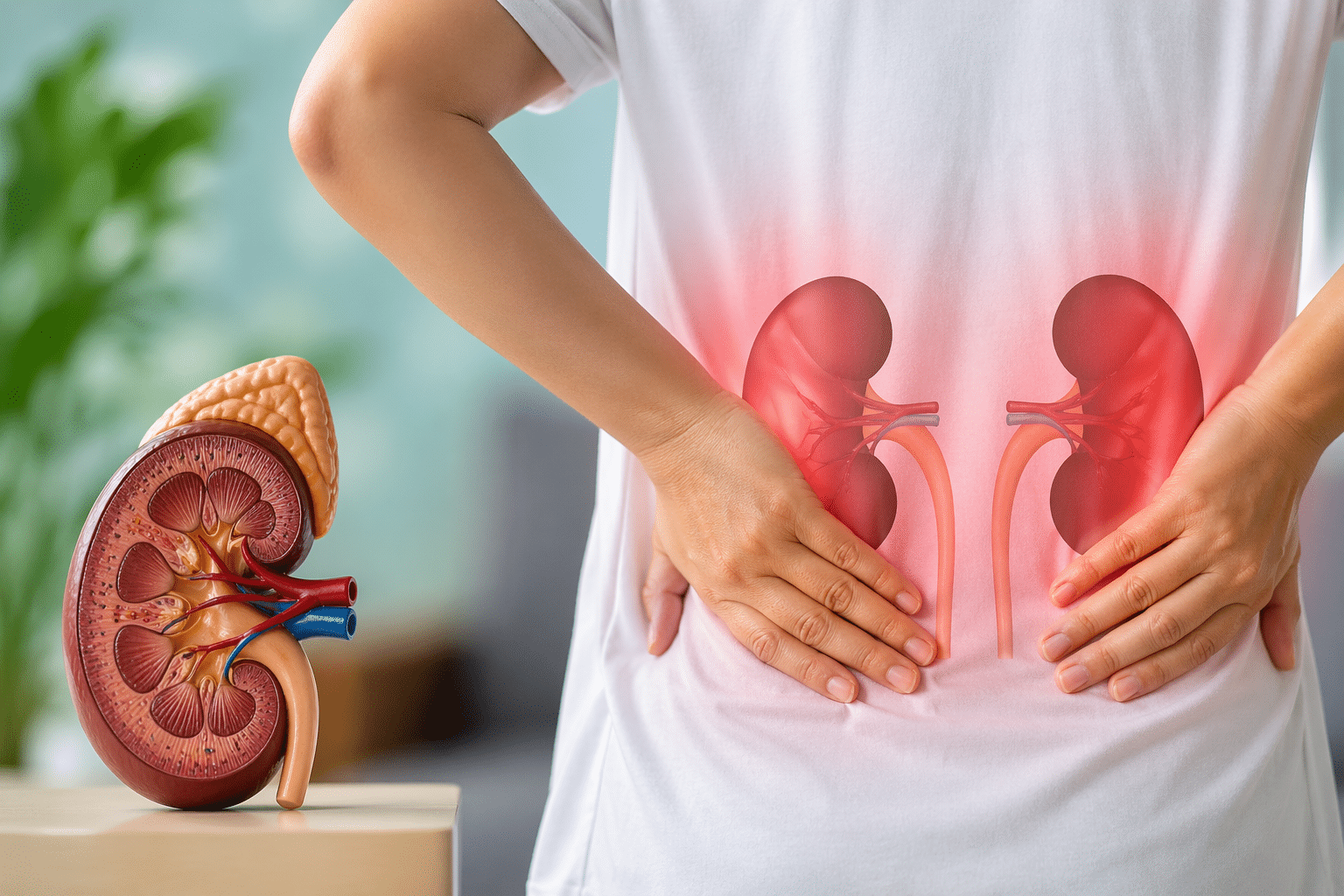
Leprosy, once a disease confined to history books, is experiencing an unexpected resurgence in the United States, particularly in Florida. With 159 cases reported in 2020 alone, this ancient disease’s modern manifestation has become a pressing public health concern. This post aims to explore the resurgence of leprosy, delve into the new cases, and discuss the public health response, shedding light on what this means for society today.
The Resurgence Of Leprosy In The U.S.

The resurgence of leprosy in the U.S. is a complex phenomenon that has been gradually building since the 1980s. After a significant reduction in cases through 2000, recent reports demonstrate a gradual increase, with states like Florida, California, and Texas becoming hotspots. This trend raises questions about the factors contributing to the rise and the implications for public health.
In 2020, Central Florida accounted for nearly one-fifth of reported cases in the country, making it a focal point for understanding this resurgence. The statistics reveal a pattern that requires careful examination, not only of the disease itself but also of the broader social and environmental factors. This leads to the need to take a closer look at the nature of leprosy, its symptoms, and its causes.
Understanding Leprosy: Causes And Symptoms

Leprosy, also known as Hansen’s disease, is an infectious condition caused by the bacterium Mycobacterium leprae. This insidious pathogen primarily targets the skin and peripheral nervous system, leading to a range of symptoms that can result in disfigurement and nerve damage if left untreated. The understanding of its biological nature is not merely an academic exercise; it’s a vital foundation for grappling with the disease’s resurgence.
The manifestations of leprosy are diverse, ranging from mild skin lesions to severe neurological impairment. Early diagnosis is paramount, as timely intervention can prevent permanent disabilities. With modern medicine, leprosy is curable through a regimen of antibiotics, a fact that underscores the importance of awareness and early detection in both medical communities and the public at large.
Geographic Concentration: Focus On Florida

Florida’s emergence as the epicenter of leprosy cases in the U.S. warrants a detailed examination. Central Florida’s high concentration of cases raises questions about local factors that may be contributing to the spread, such as climate, population density, and interaction with specific animal species.
Compared to other states, Florida’s situation is unique. The state’s environment and demographics may offer insights into the disease’s transmission and control. This geographic focus sets the stage for a broader discussion on transmission patterns, including the connection between leprosy and armadillos.
Transmission: Travelers And Local Cases

Historically, leprosy cases in the U.S. were often linked to travelers entering the country. However, a shift has occurred in recent years, with approximately one-third of cases from 2015 to 2020 appearing to have been acquired locally. This change in transmission dynamics indicates that leprosy is no longer confined to isolated cases from abroad but has become a domestic public health concern.
The implications of this shift are profound, as it suggests a potential change in the epidemiology of the disease. Local transmission means that new strategies may be required for prevention and control. Understanding this shift is essential for adapting public health strategies to the local context, including potential animal reservoirs like armadillos.